10 Common Forms of Birth Control & 10 Tips for Choosing the Best Contraception for You
10 Common Forms of Birth Control & 10 Tips for Choosing the Best Contraception for You
Know Your Options
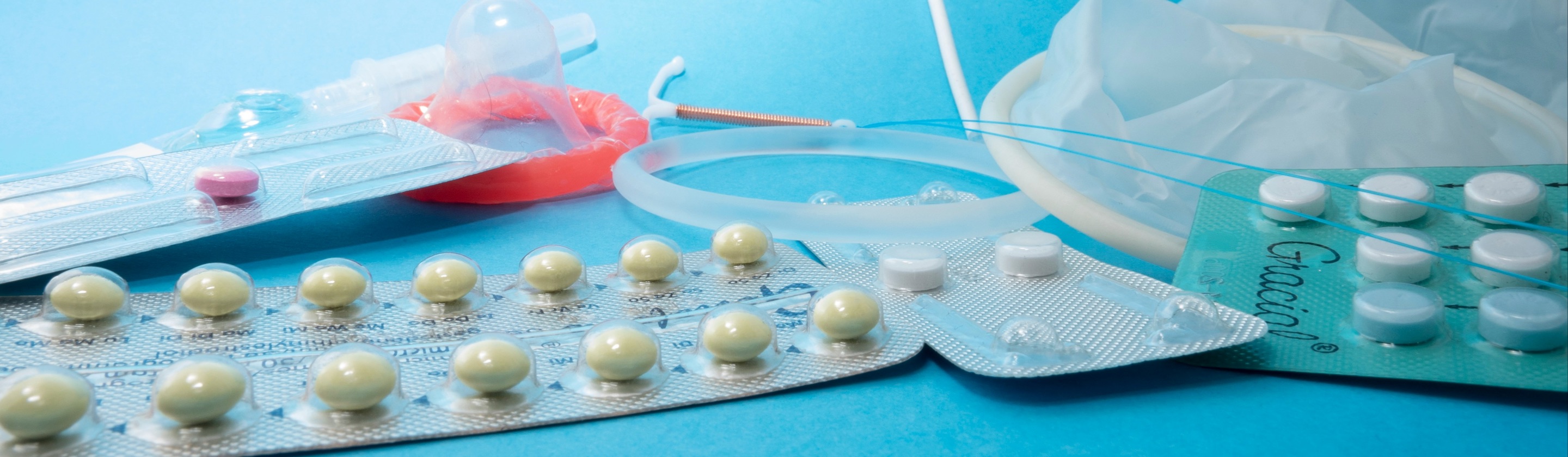
When it comes to birth control, there's no single solution that works perfectly for everyone, and understanding what's out there is the first step toward making an informed choice. Whether you're just starting to think about contraception or reconsidering what you're currently using, having a solid grasp of the most common methods can make a real difference in your confidence and peace of mind. From daily pills to long-term devices, the options are more varied than ever, and each one comes with its own set of benefits worth knowing about.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
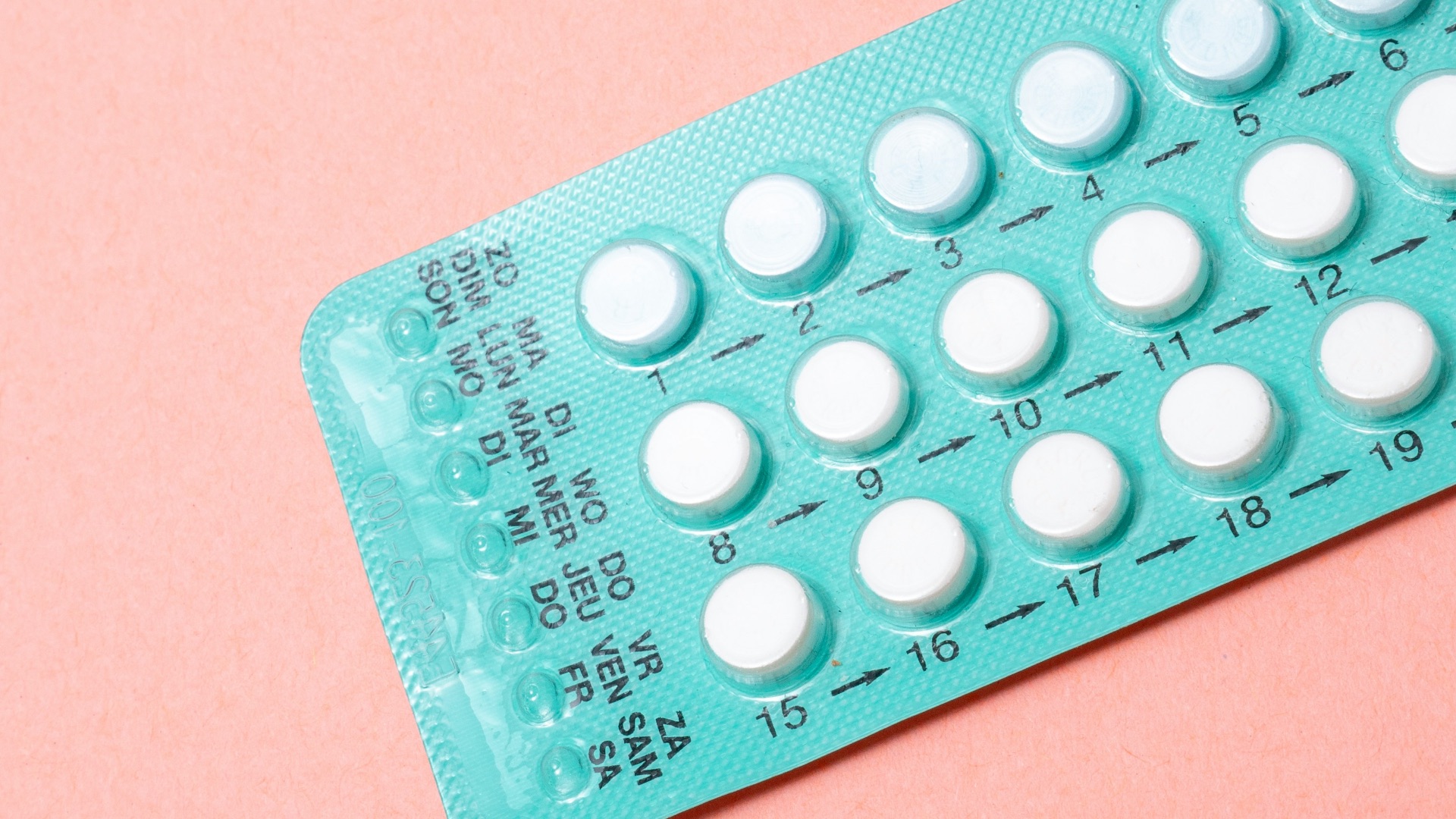
1. The Combined Oral Contraceptive Pill
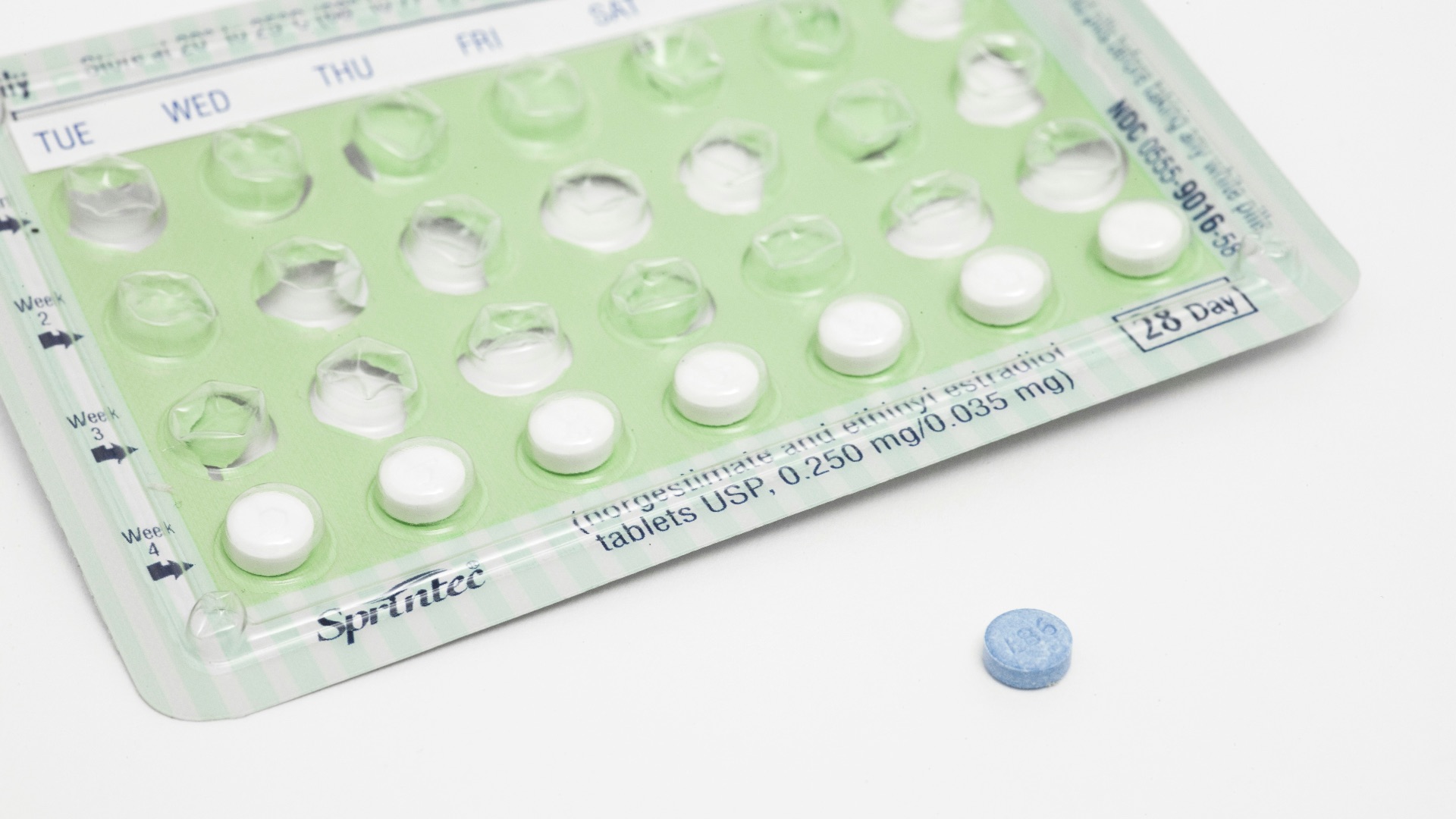
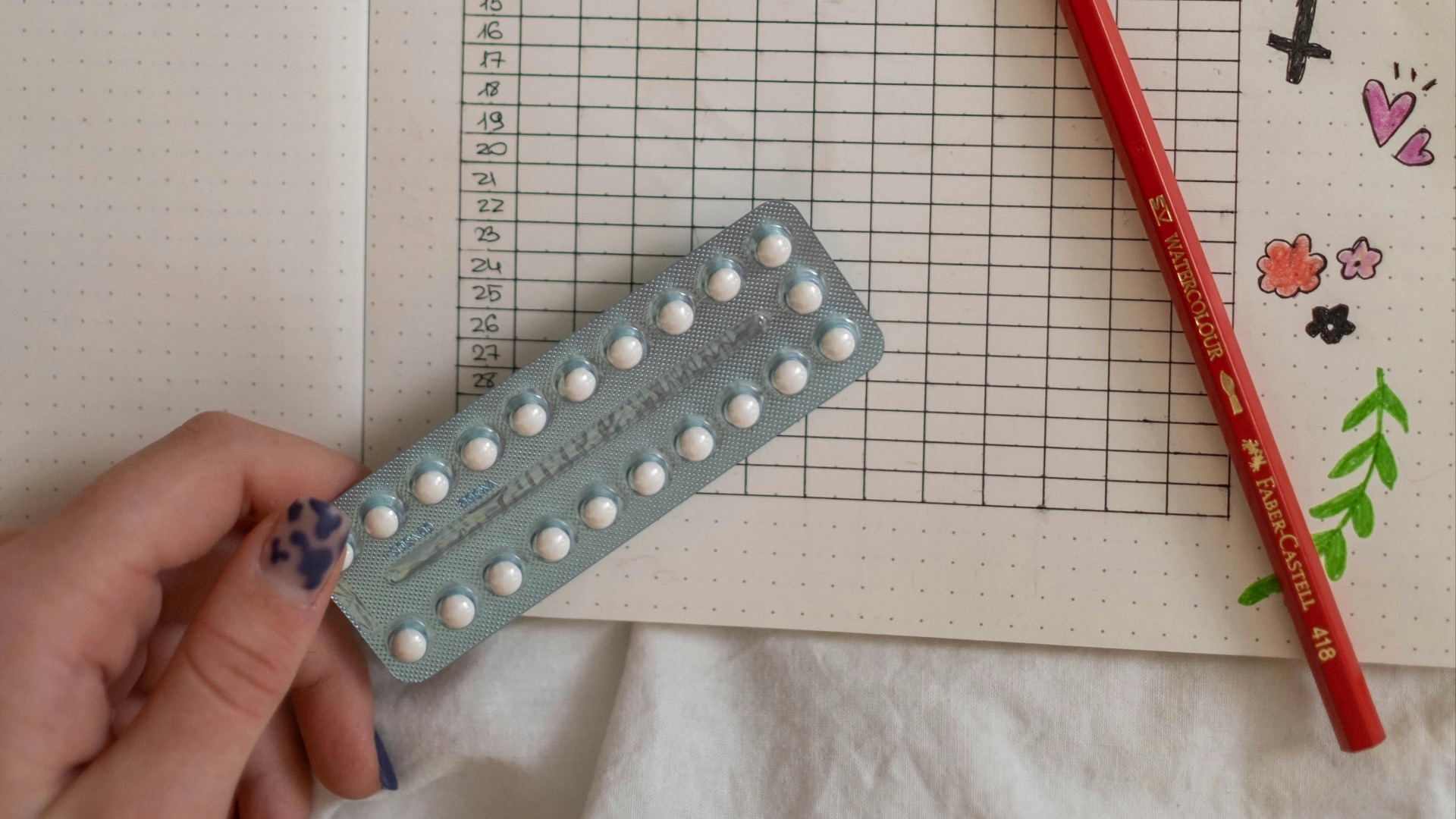
The combined pill, which contains both estrogen and progestin, works by preventing ovulation and is one of the most widely used forms of birth control in the world. It's taken daily at roughly the same time each day, and when used correctly, it's over 99% effective at preventing pregnancy. Beyond contraception, many people find that it also helps regulate their menstrual cycle and reduces period pain.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
2. The Progestin-Only Pill (Mini-Pill)
The mini-pill is a great alternative for those who can't take estrogen, including people who are breastfeeding or who have certain health conditions that make combined pills unsuitable. It works primarily by thickening cervical mucus to prevent sperm from reaching an egg, and it requires strict timing since it has a narrower window for daily use. It's just as effective as the combined pill when taken correctly, so it's a solid option if your healthcare provider recommends avoiding estrogen.
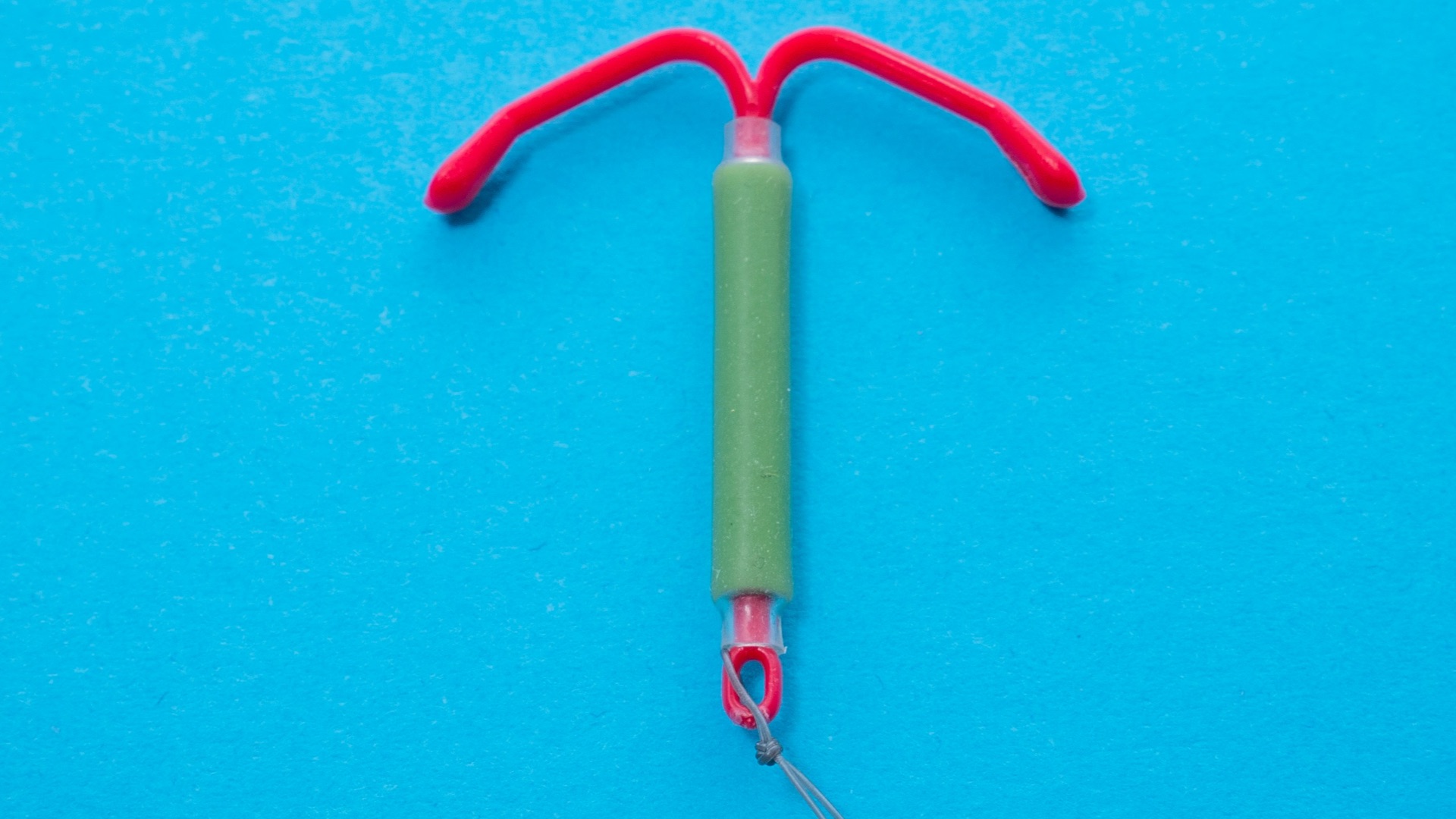
3. The Hormonal IUD
A hormonal IUD is a small, T-shaped device inserted into the uterus by a healthcare provider, where it releases low levels of progestin to prevent pregnancy. Depending on the brand, it can last anywhere from three to eight years, making it a highly convenient long-term option. Many users also experience lighter periods or none at all over time, which is a welcome bonus for those who deal with heavy or painful cycles.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
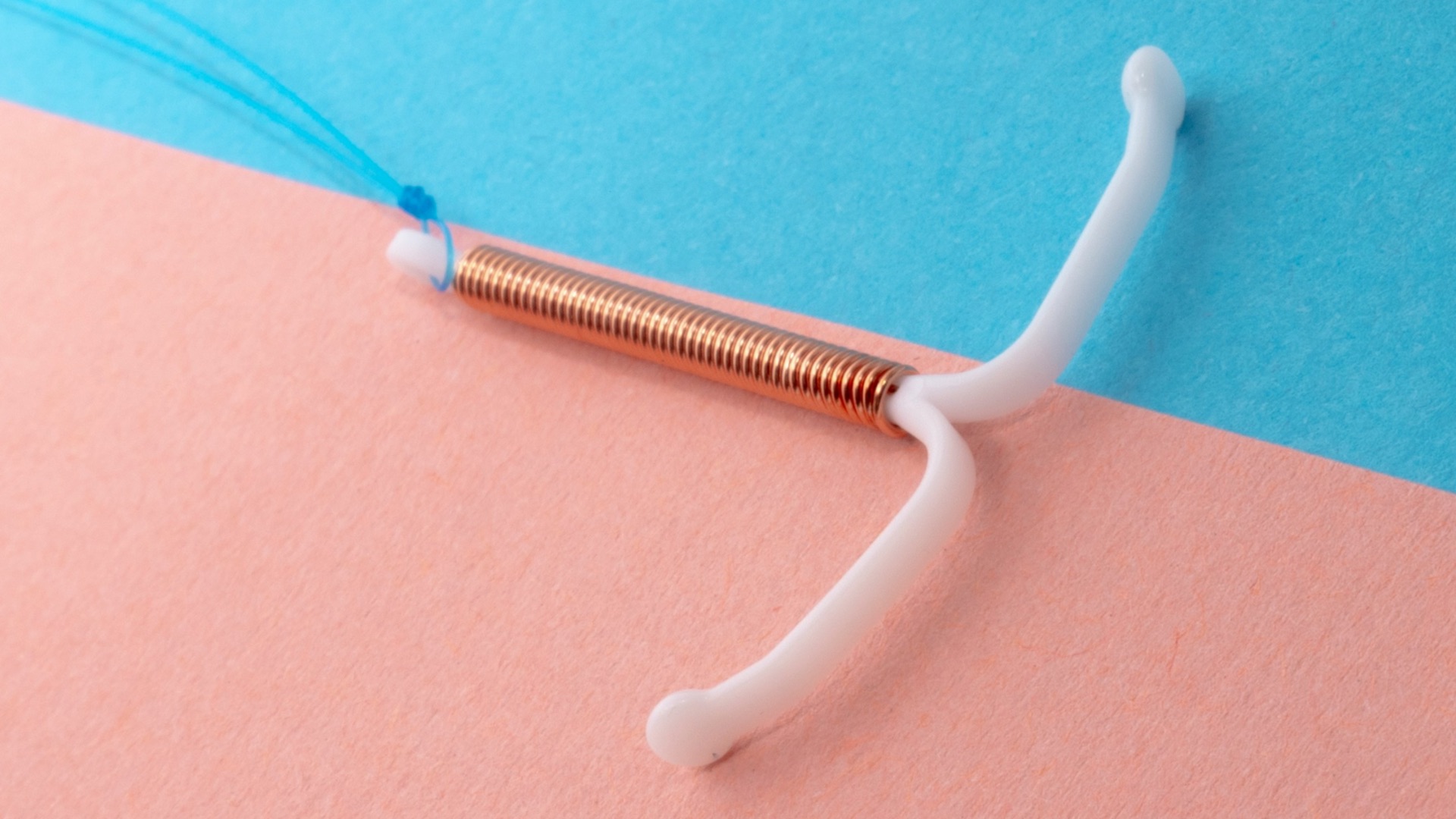
4. The Copper IUD
Unlike its hormonal counterpart, the copper IUD is completely hormone-free, which makes it a popular choice for those who prefer to avoid hormonal contraception altogether. It works by releasing copper ions that are toxic to sperm, and it's over 99% effective, making it one of the most reliable methods available. It can also be used as emergency contraception if inserted within five days of unprotected intercourse.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
5. The Contraceptive Implant
The implant is a thin, flexible rod inserted under the skin of your upper arm that releases progestin to prevent pregnancy for up to three to five years. It's one of the most effective forms of contraception available, with a failure rate of less than 1%, and you don't have to think about it once it's in place. Insertion and removal are both quick in-office procedures, so it's a relatively low-commitment way to get long-term protection.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
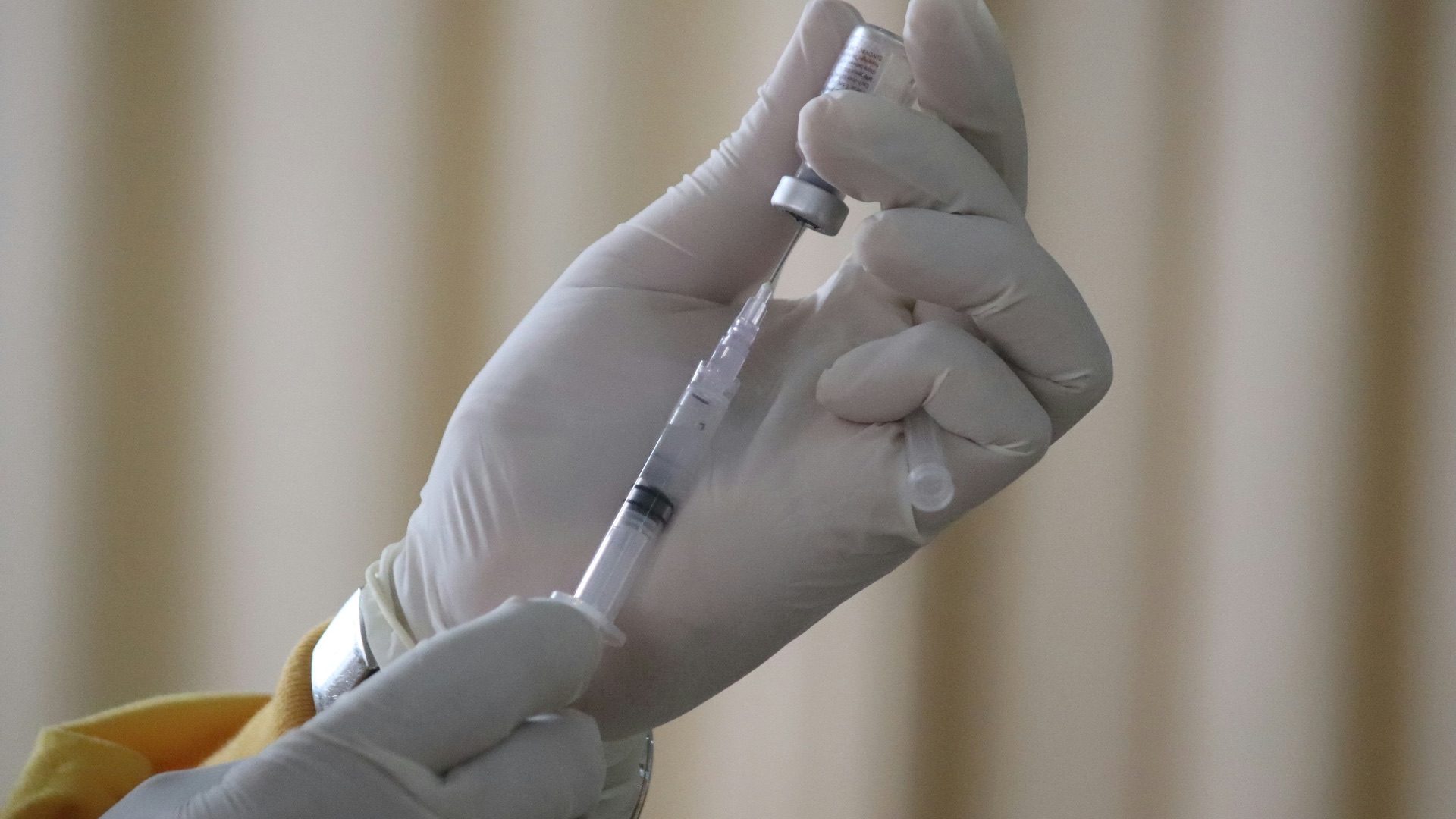
6. The Injectable Contraceptive
Contraceptive injections, most commonly known by the brand name Depo-Provera, deliver a dose of progestin every three months to prevent ovulation. They're a convenient choice for anyone who doesn't want to take a daily pill but isn't quite ready for a longer-term device like an IUD or implant. It's worth noting that fertility can take several months to return after stopping injections, so this is something to factor in if you're considering future pregnancy.
7. The Contraceptive Patch
The patch is a small adhesive square you wear on your skin that releases estrogen and progestin into the bloodstream to prevent pregnancy. You replace it once a week for three weeks, then go patch-free for the fourth week, making it a manageable routine for those who find daily pill-taking tricky to keep up with. It's similarly effective to the combined pill and is a solid middle ground between short-term and longer-term methods.
 James Heilman, MD on Wikimedia
James Heilman, MD on Wikimedia
8. The Ring
Sold under brands like NuvaRing, this flexible ring is inserted once a month to release a steady dose of estrogen and progestin. It stays in place for three weeks before being removed for a week, and because the hormones are absorbed locally, it delivers a lower overall dose than some other hormonal methods. It's discreet, easy to use once you're comfortable with insertion, and highly effective when used as directed.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
9. Condoms
Condoms are the only form of contraception that also protects against transmitted infections, which makes them uniquely valuable compared to other methods. When used correctly and consistently, condoms are about 98% effective, and they're readily available without a prescription.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
10. Permanent Contraception
Permanent contraception is intended for those who are certain they don't want future pregnancies. Tubal ligation, commonly referred to as "getting your tubes tied," involves surgically blocking, cutting, or removing the fallopian tubes to prevent eggs from reaching the uterus. This procedure is highly effective and largely irreversible, so they're best suited for people who've given the decision careful, long-term thought.
Now that you have a clearer picture of what's available, the next step is figuring out which method actually makes sense for your life. Here are ten practical tips to help you narrow it down.
1. Consider Your Health History
Some contraceptive methods aren't suitable for everyone, and your personal health history plays a big role in determining which ones are safe for you to use. Conditions like high blood pressure, migraines with aura, or a history of blood clots can rule out estrogen-based methods, so it's important to be upfront with your doctor about your full medical background. A thorough conversation with a healthcare provider is always the best starting point.
2. Think About How Long You Want Protection
Your timeline matters when choosing a method, since some options are designed for short-term use while others can provide protection for up to a decade. If you're not planning a pregnancy anytime soon, a long-acting reversible option like an IUD or implant might offer the kind of worry-free coverage that fits your life best. On the other hand, if your plans are less certain, a method with quicker reversibility might be a better fit.
3. Factor in How Often You Want to Think About It
Some people are great at taking a daily pill at the same time every day, while others find it difficult to keep up with a strict routine. If remembering a daily medication feels like a stretch, methods like the patch, ring, injection, or long-acting devices remove the day-to-day responsibility. Being realistic about your habits is one of the most practical things you can do when choosing a contraceptive.
4. Talk to Your Healthcare Provider About Side Effects
Every method carries the possibility of side effects, and what one person tolerates easily might not work well for someone else. Hormonal methods can sometimes affect mood, libido, or skin, though many people experience no significant changes at all. Your provider can help you understand what to expect and suggest alternatives if something isn't working for you after a trial period.
5. Don't Overlook Cost and Accessibility
Affordability and access are practical realities that affect which methods are actually viable for you. Some long-acting methods have a higher upfront cost but work out to be more cost-effective over time, while others, like the pill or condoms, are easier to access on a month-to-month basis. Checking what your insurance covers, or looking into local health clinics that offer subsidized contraception, can open up more options than you might expect.
6. Decide Whether STI Protection Matters to You
If you're not in a mutually monogamous relationship or if STI prevention is a priority for you, it's worth keeping in mind that most forms of contraception don't offer any protection against infections. Condoms are the only widely available method that reduces STI transmission, and healthcare providers recommend using them alongside another form of contraception for dual protection.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
7. Reflect on Whether You Want to Avoid Hormones
Hormonal contraception works very well for many people, but some prefer to avoid it for personal, medical, or lifestyle reasons. Non-hormonal options like the copper IUD, condoms, and fertility awareness methods are all worth exploring if this is a priority for you. Being clear about your preferences from the start helps your provider point you toward the right options more quickly.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
8. Know That It's Okay to Switch
Choosing a contraceptive method isn't a permanent decision, and it's completely normal to try something and realize it's not quite right for you. Your needs and circumstances will change over time, and your birth control should be able to adapt along with them. If something isn't working for you physically or practically, bring it up with your provider sooner rather than later.
 Reproductive Health Supplies Coalition on Unsplash
Reproductive Health Supplies Coalition on Unsplash
9. Involve Your Partner in the Conversation
Contraception is often thought of as a solo decision, but if you're in a relationship, having an open conversation with your partner about preferences and expectations can be really helpful. Some people prefer to share the responsibility, which might mean incorporating methods like condoms or discussing whether a vasectomy or tubal ligation is something either of you wants to consider longer-term. A shared approach tends to lead to more consistent and comfortable use overall.
10. Trust Your Instincts and Revisit Your Choice Regularly
Even after you've done your research and spoken to a provider, your own comfort and confidence with a method matter more than any data point. If something doesn't feel right for your body or your lifestyle after giving it a fair try, that's worth taking seriously and discussing with a professional. Revisiting your contraceptive choice every year or two, or after any major life change, is a smart habit to keep up with your overall reproductive health.
KEEP ON READING

10 Pre-Workout & 10 Post-Workout Tips To Follow